Managing the unmentionable
August 16, 2015, Sunday Peter Tan, mail@petertan.com
THERE are some aspects of impairments that disabled people don’t discuss openly, even with each other.
Two of them are the lack of bladder and bowel control. More than often, we shy away from talking about them, perhaps due to the private nature of the matters or maybe because the mention of them sounds disgusting.
No matter how unsavoury it may be, this subject should not be taken lightly. These are crucial issues we have to deal with regardless. They could turn into life-threatening situations requiring urgent medical intervention if not managed properly.
For this week, I would like to talk about bowel management, a topic the doctors I consulted didn’t take the trouble to discuss with me in detail until I started seeing doctors specialising in rehabilitation medicine.
Most people take that activity in the toilet for granted. When a man has to go, he has to go, right? You don’t think much about it.
For those of us with spinal cord injury, spina bifida or similar conditions, it’s a different story altogether.
Apart from the loss of sensation and limb movements, we also lose control over organs that require voluntary muscle functions. Clearing our bowels is one of them.
We each have our own programme to deal with it specifically. It has to be planned and worked into a routine so that our daily activities are not interrupted. As we have lost the ability to control our bowel movements we need some assistance to keep it going regularly.
Since the very beginning, I was started on suppositories but I developed my bowel programme through trial and error without the advice from doctors.
The same programme has largely worked on me for the past 30 years but not always.
As I could not sit up for long hours initially, I would lie on my side and defecate on the bed. My mother would clean me up afterwards.
When my physical condition improved, I used the toilet. Because I have poor sensation on my buttocks, I was always mindful of the risks of getting pressure sores when sitting for too long on the hard surface of the toilet seat.
Some of my friends do it daily. I found twice a week after dinner more effective as it becomes easier when there is sufficient bulk.
It was made even easier with a daily glass of prune juice or a few preserved prunes which acted as mild laxatives. Both tasted awful and were not something I looked forward to ingesting.
When I lapsed in the routine, the consequences were dire. There was a time when I was so constipated that I broke out in cold sweat, my heart thumped and my head felt like it was about to explode.
That I later discovered were symptoms of autonomic dysreflexia. If the obstruction was not cleared immediately, it could have led to stroke, heart attack or even death.
Luckily for me, it was resolved after huffing and puffing for half an hour without the need for more extreme interventions. Nonetheless, these are symptoms disabled people have to be aware of and seek medical attention for quickly if they persist.
Autonomic dysreflexia can also be caused by distended bladder, urinary tract infection, pressure sores and a host of other problems associated with physical trauma and pain.
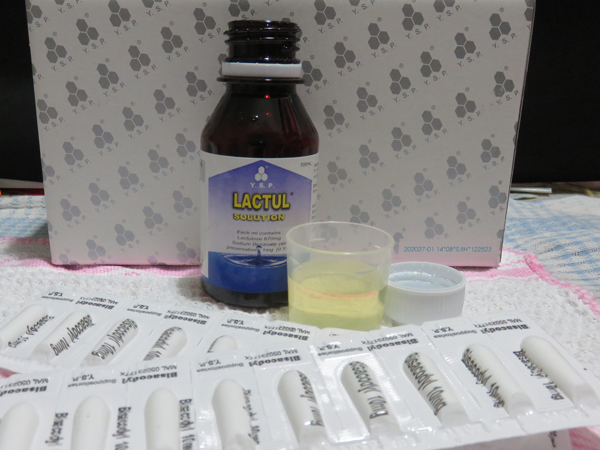
I have substituted prune juice with lactulose now. It is a synthetic sugar syrup that is broken down in the colon by gut bacteria. This process draws water from the body into the colon and softens stools. Its extreme sweetness makes it equally nauseating. The only good thing is that I only need to take one small dose daily.
In my case, suppositories and lactose are effective to a certain extent. A balanced and high fibre diet of vegetables and fruits together with adequate fluid intake are also essential in maintaining good bowel health. No punishment can be worse than sitting in the toilet for two hours without result. That is why I adhere to my bowel programme and dietary plan as best as I can.
My disabled friends have their own methods of initiating bowel movement. They either take oral laxatives or use enemas. Two other less used options are digital stimulation and digital evacuation. The former involves moving a finger lubricated with jelly in a circular motion inside the rectum to trigger bowel movement while the latter is a technique of removing faeces manually.
Whatever method practised, it is best to consult doctors who are familiar with such health conditions in order to work out a suitable bowel programme. There are advantages and disadvantages to each method depending on one’s lifestyle and preference.
I wish I was made aware of the options earlier so that I didn’t have to go through embarrassing episodes of moving my bowels at the most inopportune moment or suffer from constipation. Managing my bowels may require a little more effort but it has certainly reduced the chances of health complications and allowed me to lead a more active social life.
Read more: http://www.theborneopost.com/2015/08/16/managing-the-unmentionable/#ixzz3uMww8gjC
